Day 1 :
Keynote Forum
Marc H V Van Regenmortel
University of Strasbourg, France
Keynote: Immune correlates of protection in individuals immunized with HIV cannot help to solve the inverse problem of inducing a protecting anti-HIV immune response in humans
Time : 10:05-10:45

Biography:
Marc H V Van Regenmortel has been an Emeritus CNRS Research Director at the University of Strasbourg in France since 2001. He previously held professorship appointments at several Universities in South Africa and France and was the Director of the Immunochemistry department of the CNRS Molecular Biology Institute in Strasbourg for 22 years. He is currently the Editor-in-Chief of Archives of Virology, J. Molec. Recognition and J. AIDS & Clin. Res., Associate Editor of Analytical Biochemistry, Frontiers in Immunology, J Immunol Methods and Bionomina .He has published 17 books in Virology and Immunochemistry, 400 research and review papers and co-edited with Brian Mahy for the third edition of the “Encyclopedia of Virology” published by Elsevier.
Abstract:
Most solvable scientific problems are downstream; direct problems which involve determining what are the effects that follow certain causes. In contrast, upstream, inverse problems involve determining what the causes of observed phenomena are and these are more difficult to solve because they may have several solutions or none at all. Medical diagnosis, for instance, is an inverse problem that consists in guessing the disease from some of its symptoms, while developing an HIV vaccine is an inverse problem which requires the identification of the multiple causes that sometimes allow a limited number of human immune systems to produce antibody (Ab) or cellular responses that protect against HIV infection. When the epitopes of antigens present in HIV Env glycoproteins are used for immunization, they are given the label "immunogens" which suggests that they are able to generate immune responses, in spite of the fact that they only trigger in the immunized host a series of reactions with B-cell receptors while it is actually the immune system (IS) that produces Abs. Many properties of the IS control the types of Abs that are produced, for instance the host Ab gene repertoire, the presence of helper and suppressor T cells, self-tolerance and numerous other immunoregulatory mechanisms in the host . Unfortunately, vaccine designers using the structure-based reverse vaccinology approach tended to ignore these factors because they focused their attention only on the recognition process between a single HIV epitope and one neutralizing MAb, expecting that an antigenic epitope would also be a good immunogen. As a result, they never succeeded in developing an effective HIV vaccine. Subsequently, a major research effort was undertaken to determine the innumerable antibody maturation pathways that lead from germline Abs to neutralizing Abs, but this also did not solve the inverse problem. In recent years, it has become widely believed that in vivo empirical immunogenicity experiments could be the only way to try to solve the inverse problem of how to induce protective immunity against HIV infection by vaccinating humans.
Keynote Forum
Kevin M Galalae
Center of Global Consciousness, Canada
Keynote: Increase fear to decrease growth: strategies of population control in an over populated world
Time : 11:00-11:40

Biography:
Kevin M Galalae is the world’s foremost independent authority on the globalization-depopulation axis around which the international system has revolved since the inception of the USA in 1945, and the first to expose and scientifically demonstrate the existence, methods and consequences of the Global Depopulation Policy. He is the Founder and Director of the Center of Global Consciousness (CGC), which is dedicated to the eradication of all covert chemical, biological, psychosocial and economic methods of population control and to their replacement with overt population control legislation through a global replacement level fertility law.
Abstract:
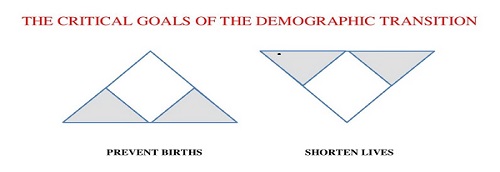
- HIV/AIDS, STDs & STIs
Session Introduction
Mohammad Akram Randhawa
Northern Border University, Saudi Arabia
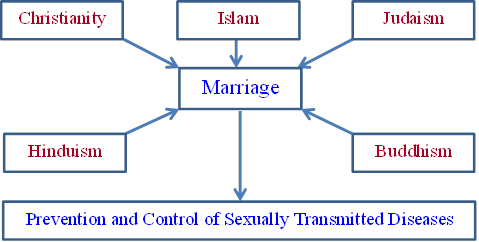
Title: Religions and marriage for the prevention and control of sexually transmitted diseases
Biography:
Abstract:
Gabriela Gore-Gorszewska
Jagiellonian University, Poland
Title: Competent sexual education as a potential STI prevention method. Reflections on ideas from across Europe
Time : 12:10-12:40

Biography:
Abstract:
Joan J Rugemalila
Muhimbili National Hospital, Tanzania
Title: Predictors associated with moderate to severe chronic kidney disease among HIV infected adult patients in Dar es Salaam, Tanzania
Time : 12:40-13:10

Biography:
Abstract:
Vera Ketty
Hospital Matilde Hidalgo de Procel, Ecuador
Title: The high seroreversion of Human Immunodeficiency Virus in vertically exposed infants who received all the care measures to reduce the mother-to-child transmission in Guayaquil, Ecuador
Time : 13:10-13:40
Biography:
Abstract:
- Public Awareness on STDS
Session Introduction
Chloe Chan
New York University, USA
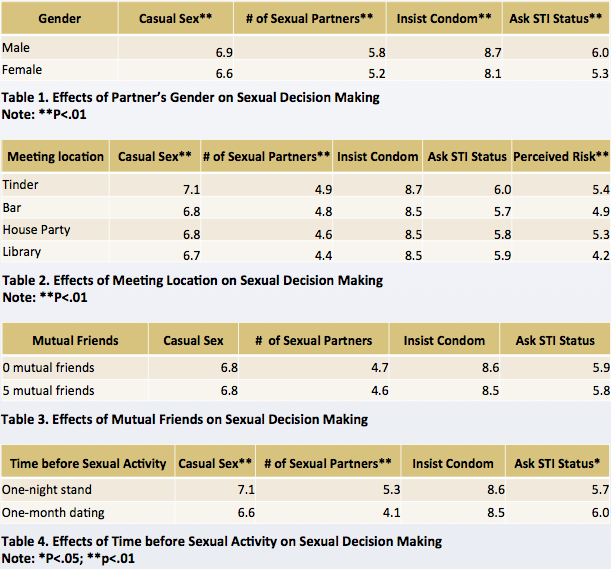
Title: The effects of contextual factors and dating app usage on sexual risk behaviors among young adults
Biography:
Abstract:
Patricia Garcia de Olalla
Public Health Agency of Barcelona, Spain
Title: Does the high prevalence of late presentation of HIV infection persist?
Biography:
Abstract:
Biography:
Abstract:
Gesesew Hailay
Flinders University, Australia
Title: HIV care continuum outcomes: does Ethiopia meet the UNAIDS 90-90-90 targets?

